by Dr. Alicia Nolfi
Laminitis is caused by many things. Any condition involving generalized infection or inflammation can cause laminitis. Pneumonia, colitis, placentitis and endometritis are some examples. Elevated simple sugar intake either over time on lush pasture, or in one occurence such as the grain overload, can cause laminitis. Full weight bearing on one limb due to an injury on the opposite limb can result in supporting-limb laminitis. One of the most common causes of laminitis is enocrine-associated and metabolic-associated. Equine Pituitary Pars Intermedia Dysfunction, otherwise known as Equine Cushing’s Syndrome, and Equine Metabolic Syndrome both are associated with a high risk of laminitis due to hyperinsulinemia (high blood insulin) that occurs and the often times state of high blood sugar in the horse. The exact cellular and chemical mechanisms that trigger laminitis due to all causes are not fully understood, although The Laminitis Institute at the University of Pennsylvania’s New Bolton Center is hard at work to help us better understand laminitis pathogenesis.
The horse foot can withstand great stresses associated with galloping and jumping, however the anatomy is complex and even delicate. The lamellae of the foot is a blood and nerve filled connective tissue structure that serves to attach the bone of the foot, the distal phalynx or coffin bone, to the hoof wall. The lamellae is arranged in a folded, acordion-like architecture that runs lengthwise from the coronary band area to the ground. There are 550-600 of these lamellae in each foot, visible to the naked eye. From each individual primary lamellae, 150-200 microscopic secondary lamella project in a perpendicular direction. These microscopic secondary and and macroscopic primary lamellae interdigitate (lock together) with the inside of the hoof wall that has a similar, matching architecture. Laminitis affects the primary and secondary lamellae, resulting in a structural failure of the attachment between the lamellae and the hoof wall, and a horse can fall anywhere on a spectrum of mild to severe laminitis related tissue damage. Seldom does laminitis affect two horses the same. Furthermore, feet are rarely affected the same on each horse even when the same podiatry and treatment regime are used. A horse can have laminitis in one foot, two feet, three feet or all four.
IMPORTANT POINT!
Regardless of the inciting cause, the condiditon of laminitis results in decreased perfusion, or blood filling of tissues, in the foot.
Laminitis prevention is vital. As with any other disease syndrome, prevention is worth a pound of cure. Recognizing the risk of laminitis in a horse and enacting a detailed and aggressive plan in an attempt to prevent its development is advantageous to waiting for laminitis to happen. Once a horse is exhibiting signs of laminitis, damage has already occured. Often times, treatment is needed for existing laminitis. The basis of treatment of the laminitis horse relies on correcting the initiating disease process, medically managing the pain of the horse, and mechanically altering the “mechanics” of the hoof to place it in a healing mode. This means establishing optimal perfusion in the foot to optimize the healing environment. Like any other organ in the body, without adequate perfusion, damage and death to cells is iminent. Laminitis should be regarded as an emergency because it is just that – lack of blood in the foot. A good analogy is having a “heart attack” in the foot. Waiting for that foot “heart attack” to happen and if it does happen, giving a little Bute and waiting to see how the horse does only decreases the chances of having a functional and comfortable horse, whether that means performace or pasture companion. This can be likened to you having a heart attack and deciding to take some Advil for the discomfort and “wait and see” what happens. Prevention and treatment strategies are often similar – maintain optimal perfusion of the foot and address underlying causes.
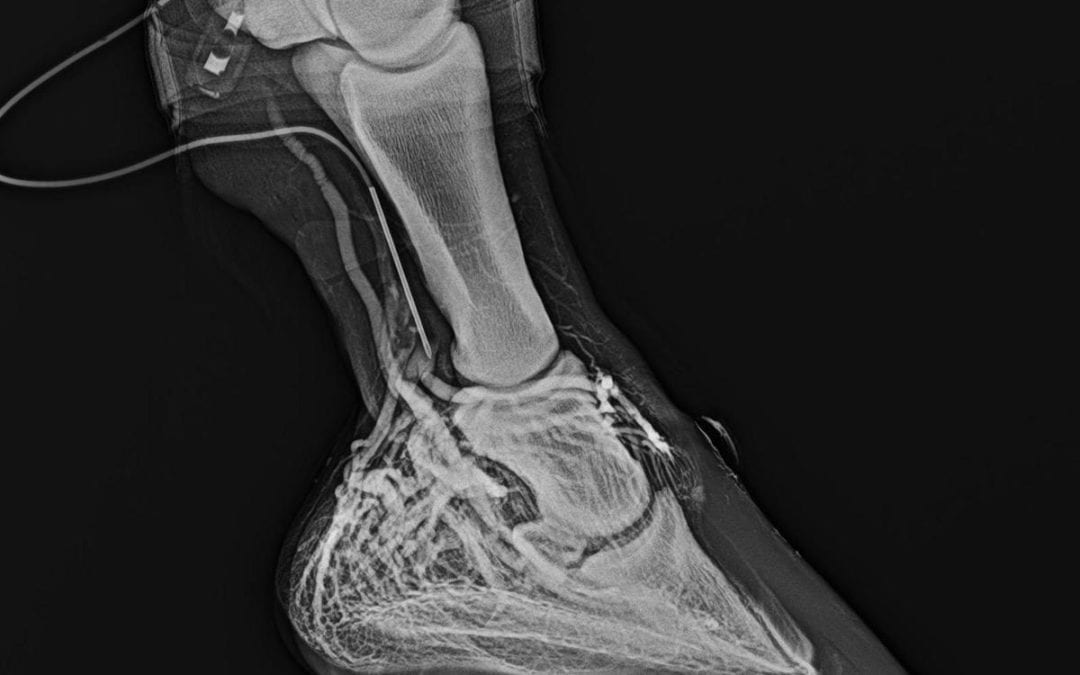
To diagnose and monitor existing laminitis and to monitor perfusion of the foot during prevention-oriented therapy of the foot, we use a diagnostic tool called the venogram. The venogram consists of xrays taken of the foot after contrast dye has been injected into the blood vessels of the foot, and evaluation of these images. Plain xray images are also an important diagnostic standard, as they allow us to measure soft tissue parameters such as sole depth, horn/lamellar zone, digital breakover and palmar/plantar angle. Plain radiographs furthermore enable us to get a good look at bone health. The major difference between plain xrays and the venogram (other than the specific types of tissues we study in each) is that plain radiographic changes, as a general rule, take much longer to develop than perfusion changes. Perfusion changes happen immediately and we can assess degree of damage on day one with the venogram. This gives us sigificant opportunity to do something NOW instead of waiting. With the venogram we can make a better estimate of prognosis (clinical lameness is only accurate in approximately 50% of cases and other prognostic parameters that people have studied have also proven unreliable), and can frequently monitor tissue damage. If our treaments are not working, we can make adjustments today, not in two or four weeks. This includes the ability to assess our shoeing mechanics treatment and determine potential or current effectiveness – on day one and at any time along the treatment process.
Laminitis does not have to be a death sentence. Together we can strive to prevent and treat laminitis in our horses in a manner that will reduce the potential for career-ending or life-threatening laminitic damage to the foot. Be aggressive!
WHAT TO DO IF YOU THINK YOUR HORSE MAY HAVE LAMINITIS:
When your horse shows clinical signs of laminitis, damage to the hoof architecture has already occurred. How you respond to these signs will help determine the course of the disease.
1. Limit the movement of the horse!!! Ignore old thoughts of walking the horse to “increase the circulation.” Movement will further damage the architecture of the hoof.
2. Research suggests that standing a horse in an ice water bath up to its knees and hocks will reduce blood flow to the feet, and perhaps prevent the trigger factors from reaching the feet. Standing a horse in an ice bath PRIOR to the development of lameness may PREVENT laminitis from occurring. Standing a horse in icy water AFTER the development of lameness reduces blood flow to tissues which need to repair and may be contraindicated.
3. Support the foot! Styrofoam insulation cut to fit the foot will help support the sole surface until help arrives.
4. Call your veterinarian and farrier, IMMEDIATELY. Acute laminitis, and acute on chronic laminitis are true emergencies. The successful outcome of a laminitis case requires a team effort be made by three individuals: the veterinarian, farrier and horse owner. If any one of the members of this team is not willing to give a 100% effort, success will be compromised. In acute cases, time is of the essence.
The guidelines listed for horseowners was developed by Dr. Amy Rucker, and much of the information contained in this article is the result of years of research, studies and clinical cases from Dr. Chris Pollitt, Dr. Ric Redden, Dr. Sammy Pittman and Dr. Amy Rucker. Thank you to all of them, and many others, for their dedication to the horse foot, and to the horses that have had laminitis that survived or have passed on that we have been so fortunate to learn from.
JOIN US FOR MORE INFORMATION ON THIS VERY IMPORTANT TOPIC
Our second program in the Equine Foot Educational Series will cover LAMINITIS! August 9, 6pm, at Rumble Ridge Ranch. See you there!